Transmission Protection When Treating COVID-19 Patients with High Velocity Therapy
All respiratory support modalities generate aerosol. However, not all of them present the same risk of nosocomial transmission. This is often reflected in guidelines from healthcare institutions. For example, the Society of Critical Care Medicine (SCCM) recommends the use of high flow oxygen as a front-line therapy over the use of NiPPV for COVID-19 patients not requiring intubation. This recommendation — Surviving Sepsis Campaign COVID-19 Guidelines — states: “patients may find HFNC more comfortable than NIPPV. Given the evidence for a decreased risk of intubation with HFNC compared with NIPPV in acute hypoxemic respiratory failure and studies suggesting that NIPPV may carry a greater risk of nosocomial infection of healthcare providers, we suggest HFNC over NIPPV.”
As a mask-free modality that delivers high flows of oxygen to patients, Vapotherm high velocity therapy has a low risk of transmission by comparison to NiPPV.[1,2,3] Nevertheless, given the infectiousness of this novel coronavirus the already low risk can and should be further reduced with a few simple precautions.
Personal Protective Equipment (PPE)
The World Health Organization (WHO) and the Centers for Disease Control (CDC) recommendations include the proper use of PPE for healthcare workers such as a N95 or equivalent respirator, gloves, and gowns among other equipment.
They also recommend performing procedures in an adequately ventilated room, preferably an Airborne Infection Isolation Room (AIIR) or Negative Pressure room.
Additional Recommendations for High Velocity Therapy
To reduce transmission risk, healthcare workers should apply a surgical mask over the nose and mouth of a patient with a properly fitted cannula before initiating therapy. New computational fluid dynamics modeling (CFD) conducted by Vapotherm’s science team shows such use of a surgical face mask greatly reduces the spread of potentially infectious particles during high velocity treatment. This CFD data follows on prior research that found the risk of transmission from high velocity therapy to be low by comparison to other ventilatory support modalities.
Figure 1 shows a velocity map of how high velocity treatment with a surgical mask compares to breathing without treatment while wearing a surgical mask.
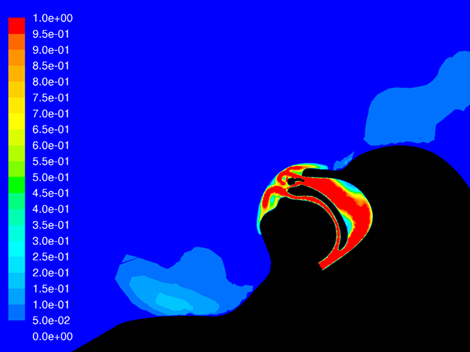

Figure 1. Particle dispersion during breathing with mask (left) and during high velocity therapy with mask (right)
The red coloring indicates a higher velocity of flow coming out of the patient’s nose and mouth. It’s apparent that the patient on high velocity therapy has a greater velocity of flow than the normal-breathing model, but it’s also apparent that this flow is being captured by the mask. Lower velocity gas flow will provide less force to particles which do leave the mask.
The authors recommend minimizing mask leakage to further reduce the risk of transmission. This recommendation is also in line with the guidance of the Respiratory Care Committee of the Chinese Thoracic Society.[4]
The Transmission Assessment Report that details the CFD results also notes that the use of the mask does not eliminate the clinical efficacy of high velocity therapy. High velocity therapy is effective in providing oxygenation support as well as ventilatory support and is a form of Mask-Free NIV™ for spontaneously breathing patients.
Visit our COVID-19 Resource Center for up-to-date answers to additional frequently asked questions.
REFERENCES
[1] Clinical management of severe acute respiratory infection when novel coronavirus (2019-nCoV) infection is suspected: Interim Guide, Page 6 January 28 2020.
[2] Leung CCH, Joynt GM, Gomersall CD, et al. Comparison of high-flow nasal canula versus oxygen face mask for environmental bacterial pneumonia patients, a randomized controlled crossover trial. J Hosp Infect 2019: 101:84-87.
[3] Hui DS, Chow BK, Lo T, et al. Exhaled air dispersion during high-flow nasal cannula therapy versus CPAP via different masks, Eur Respir J 2019,53.
[4] Respiratory care committee of Chinese Thoracic S. [Expert consensus on preventing nosocomial transmission during respiratory care for critically ill patients infected by 2019 novel coronavirus pneumonia]. Zhonghua jie he he hu xi za zhi = Zhonghua jiehe he huxi zazhi = Chinese journal of tuberculosis and respiratory diseases. 2020;17(0):E020.