Vapotherm Blog
CAUTION: US Federal law restricts this device to sale by or on the order of a physician. Indications, contraindications, warnings, and instructions for use can be found in the product labelling supplied with each device or at https://vapotherm.com/resources/support/precision-flow-reference/. For spontaneously breathing patients. High Velocity Therapy (HVT) does not provide total ventilatory requirements of the patient. It is not a ventilator. Decisions surrounding patient care depend on the physician’s professional judgment in consideration of all available information for the individual case, including escalation of care depending on patient condition.
Vapotherm provides high velocity nasal insufflation (HVNI) with simultaneous oxygen delivery to augment breathing of spontaneously breathing patients suffering from respiratory distress and/or hypoxemia in the hospital setting. It is not intended to provide total ventilatory requirements of the patient and not for use during field transport.
The information provided in this section is for educational purposes only. This information is not intended to support the safety or effectiveness of Vapotherm products, or diagnose, treat, cure, or prevent any disease. It is not a substitute for consultation with your healthcare provider and should not be construed as medical advice.

Vapotherm to Unveil Access365 Home Ventilation Solution at MEDTRADE
Dr. Jessica Whittle, Chief Medical Officer of Vapotherm, emphasized the company’s commitment to improving the lives of hypercapnic patients in the home. “Our mission is to improve quality of life and reduce hospital readmissions for patients who struggle with respiratory disease. Access365 will provide optimal treatment at home, especially for COPD patients, by combining the known benefits of nocturnal NIV with the comfort of high velocity therapy for daytime use.”

Onymos and Vapotherm Announce Partnership to Create an End-to-End Internet of Medical Things Solution (IoMT)
Partnership enables Vapotherm to build a robust and secure solution 80% faster than the standard development timeline to meet data visualization and device management goals for HVT® 2.0 and future Home system
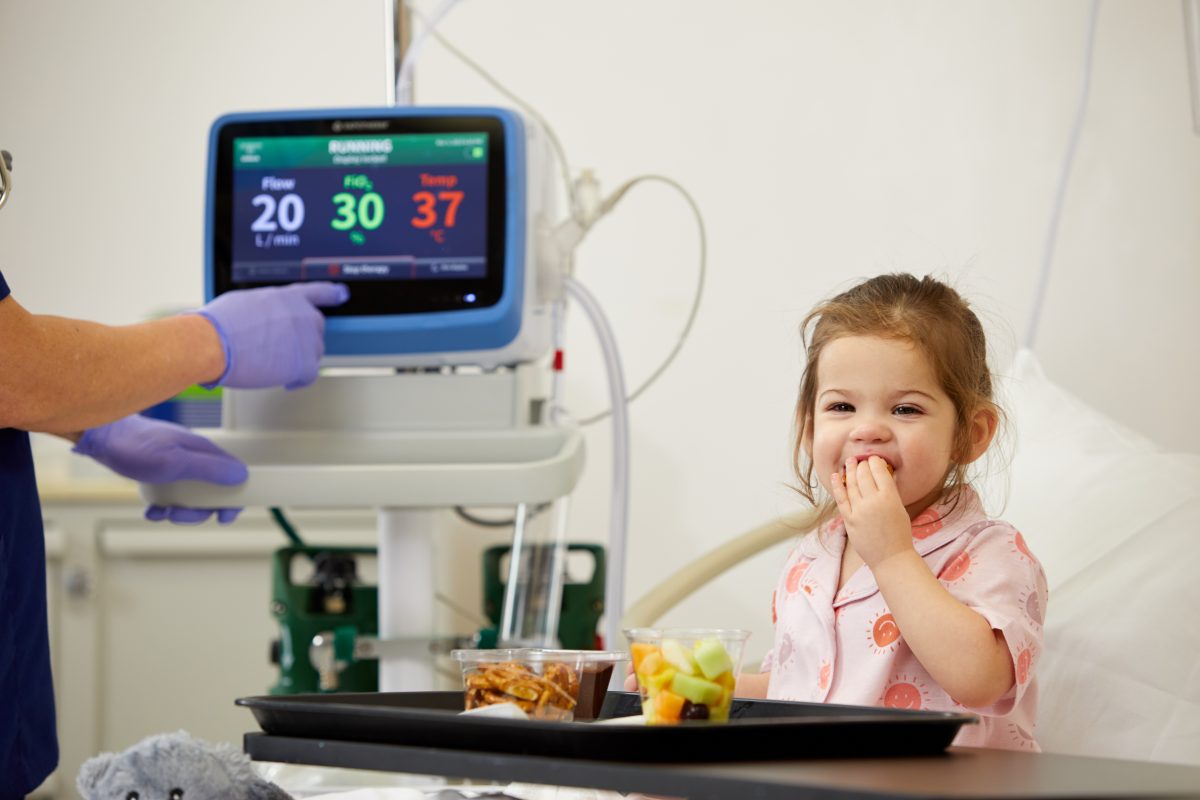
Letting Children be Children
While the advantages of early mobility in critical care are widely acknowledged, its profound impact on patient mental well-being is equally significant. Hear from this Paediatric team at Freeman Hospital, Newcastle, UK, as they share their experience on how much Vapotherm’s mobility solution positively impacts their patients and their families.

Five Benefits Vapotherm HVT 2.0 Can Offer Your Small (Sometimes Rural) Hospital
Does your hospital struggle finding a safe, effective, easy to use respiratory support option for stabilizing patients in respiratory distress? Vapotherm’s HVT 2.0 advanced respiratory support platform provides fast and effective support for your patients in respiratory distress. HVT 2.0 prioritizes safety, comfort, and convenience for both patients and clinical staff. Learn how your facility can realize these benefits by testing the performance of HVT 2.0 and assess its suitability for various patient cases with no upfront commitment through Vapotherm’s Trial Program!

Presenting HYPERACT
We invite you to learn about this recent multi-center, randomized controlled trial (RCT) which challenges the accepted standard treatment for patients with an acute exacerbation of moderate-severe COPD.

Vapotherm Interview with Shelley Rose – Helping Make Those First Cuddles Possible
Hear from Shelley on how the Vapotherm Transport solution lets you provide respiratory support at the bedside, allowing skin to skin, for full term babies who have an oxygen requirement at birth and who would have normally been admitted to the Neonatal Unit.
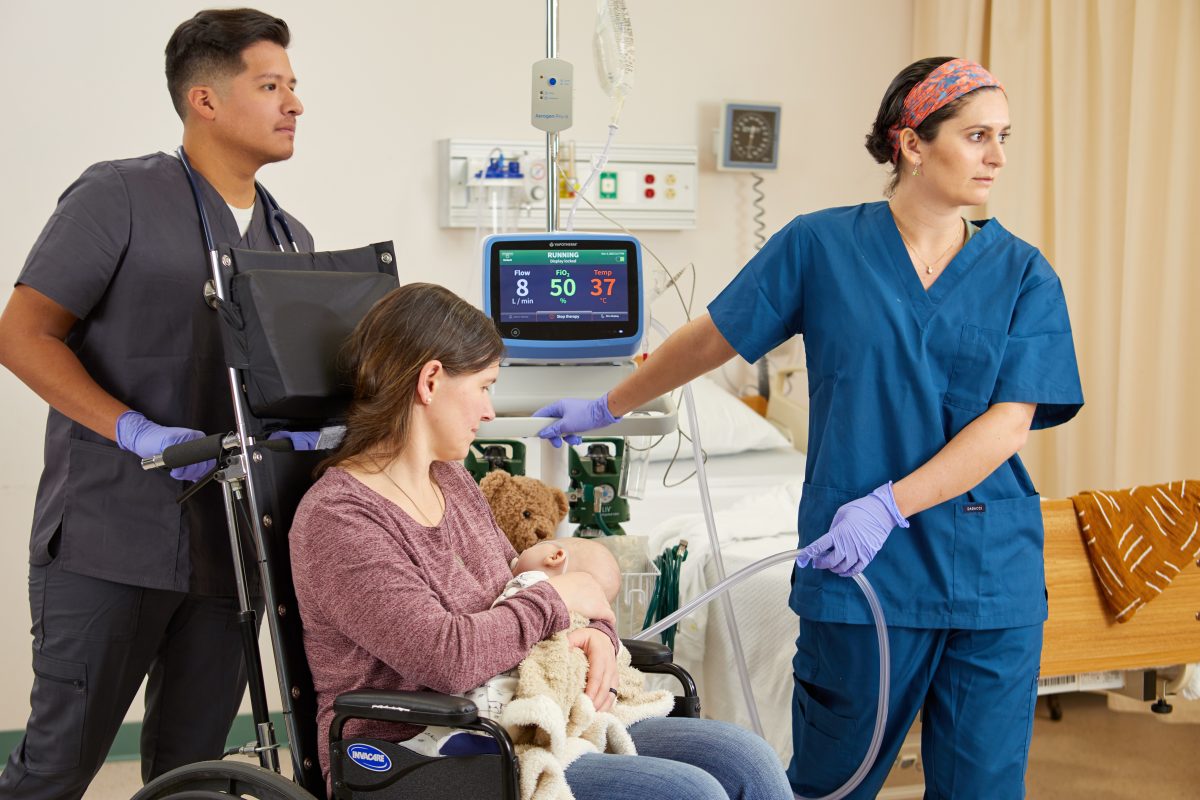
High Velocity Therapy Resources and Tools for RSV
Winter is coming. Winter, as in, Respiratory Syncytial Virus (RSV) season. Last year’s RSV season hit the US earlier and harder with a record-breaking mix of strep infections, flu, RSV, and enteroviruses to compete with COVID. According to the CDC, during the 2022 season, early epidemic onsets (April-June) were observed in Florida and some regions (New England, Georgia, Texas), however, RSV leveled off before increasing again in September. Regions more north and west (New York, Colorado, California, and Washington) experienced RSV season peak in October and November.
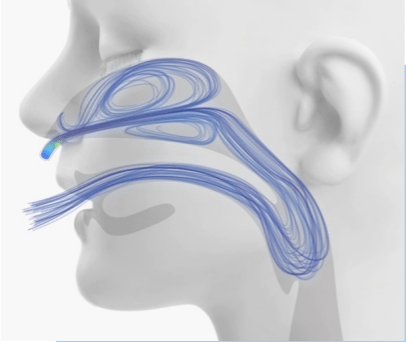
Characteristics of Flow Author Interview
Below is an interview with first author, Robert Kacinski, and senior author, Scott Leonard, on a paper that they presented at the 8th Thermal and Fluids Engineering Conference (TFEC) in May 2023 comparing flow characteristics in the upper airway with 1. no therapy, 2. high flow nasal cannula (HFNC) therapy and 3. high velocity nasal insufflation (HVNI) in different scenarios.

High Velocity Therapy and Increased Work of Breathing Roundtable
In the following Roundtable discussion, Emergency Medicine and Critical Care Physicians experts in respiratory therapy explain different applications for the system for increased work of breathing in both lung and non-lung pathology patients.

Rethinking the ABCs with Dr. Jeremy Greenberg
In this LIVE recorded presentation, Dr. Greenberg:
Reviews the impact and consequences of increased work of breathing
Describes the mechanisms of action of High Velocity Therapy
Explains the many applications of High Velocity Therapy