COVID-19 Best Practices with Vapotherm High Velocity Therapy
The last weeks have proven to be a steep learning curve for COVID-19 respiratory symptom management. Here is a quick list of best practices for Vapotherm high velocity therapy.
Remember: No Need to Intubate Everyone
When COVID-19 first broke out, the initial course of symptom management across many locales was early intubation. Given that we now know that COVID-19 patients on ventilators don’t do very well,[1,2] the clinical consensus has shifted toward first attempting support with noninvasive modalities, provided the patients don’t require immediate intubation. Most organizations across the world, including the CDC and WHO, call for monitored trials with high flow modalities, which includes Vapotherm high velocity therapy.
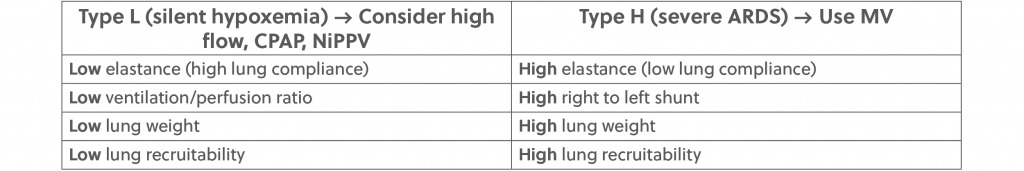
Gattinoni and colleagues have identified two phenotypes that could help clinicians decide which patients may be in need of immediate intubation (20-30%) and which ones could be successfully managed with noninvasive support (70-80%).[3] Table 1 summarizes the phenotypes.
Table 1. COVID-19 Phenotypes
Reducing Risk of Transmission to Healthcare Workers
All procedures that manipulate the airway in some shape or form are aerosol generating procedures (AGPs). However, not all AGPs carry the same transmission risk. Procedures associated with intubation have among the highest risk while high flow modalities have some of the lowest risk.[4]
Several COVID-19 clinical management guidelines, including those from the Society of Critical Care Medicine (SCCM)[5] and the Australian and New Zealand Intensive Care Society (ANZICS),[6] don’t recommend routine use of noninvasive positive pressure ventilation (NiPPV). The key concern behind this recommendation is that NiPPV may present a higher transmission risk, especially with poor mask fit, than high flow modalities.
Although high velocity therapy is a mask-free form of NIV and has similar efficacy to NiPPV, in this context of AGP and transmission risk, it is more comparable to standard high flow devices. Because of its cannula interface and high velocity (not pressure-based) mechanism of action, it has a relatively low risk of nosocomial transmission.
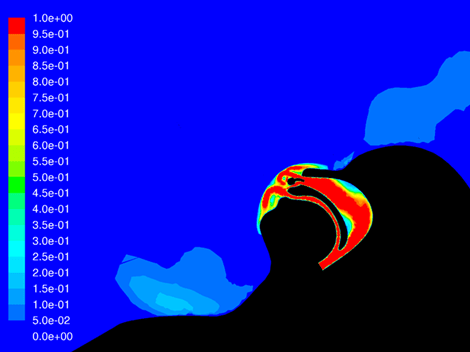
Nevertheless, healthcare providers should wear appropriate PPE and, when possible, use negative pressure rooms when treating COVID-19 patients with high velocity therapy. In addition to the standard PPE guidance, computer modeling of high velocity therapy shows that using a simple surgical mask over the high velocity therapy cannula greatly reduces the dispersion of potentially infectious particles.[7] The reduction is comparable to the dispersion seen in normally breathing patients wearing a surgical mask. Figure 1 shows a velocity map of how Vapotherm therapy treatment with a surgical mask compares to breathing without treatment while wearing a mask.
Figure 1. Particle dispersion during breathing with mask (left) and during high velocity therapy with mask (right)
Because high velocity therapy is mask-free NIV, it may be an attractive tool in patients requiring ventilatory support in addition to oxygenation support, such as COPD exacerbation patients.
The Benefits of Humidification
The airway requires nearly 100% relative humidification of inhaled gas to function optimally.[8] High velocity therapy is designed to generate optimally humidified medical grade vapor and deliver it to the patient in an energetically stable way. This may be particularly beneficial for COVID-19 patients as current recommendations for management call for the restriction of fluids under certain conditions[5] — something that could further challenge that patient’s ability to heat and humidify their airway.
Conservation of Oxygen
Some hospitals are concerned about oxygen shortages as they try to meet the demands of hypoxemic COVID-19 patients. As you develop a plan for resource management, it’s relevant to understand that Vapotherm therapy flushes the airway dead space faster than large-bore cannulas used by conventional HFNC.[9] Due to this faster flush, high velocity therapy is clinically effective at below 40L/min. Standard HFNC generally require much higher liter flows to achieve the slower flush — a distinction that is meaningful if oxygen conservation is of concern.
Using Vapotherm High Velocity Therapy for Post-Extubation Support
Some COVID-19 patients will inevitably need to be intubated. High velocity therapy may be an attractive option when considering respiratory support for post-extubation. Thille and colleagues have found that extubation success is highest when a combination of HFNC and NiPPV are used.[10]
Due to the comfortable, mask-free interface, patients can eat, drink, talk, and take oral medications while also receiving ventilatory support comparable to that of NiPPV.[11,12] This comfortable yet efficacious therapy could be an attractive option for post-extubation respiratory support, whether for COVID-19 patients or others.
Visit our COVID-19 Resource Center for up-to-date answers to additional frequently asked questions.
REFERENCES
[1] Yang X Yu Y Xu J et al. Clinical course and outcomes of critically ill patients with SARS-CoV-2 pneumonia in Wuhan, China: a single-centered, retrospective, observational study. Lancet Respir Med. 2020; (published online Feb 24.) https://doi.org/10.1016/S2213-600(20)30079-5
[2] Zhou F Yu T Du R et al. Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: a retrospective cohort study. Lancet. 2020; (published online March 9.) https://doi.org/10.1016/S0140-6736(20)30566-3
[3] Gattinoni L. et al. COVID-19 pneumonia: different respiratory treatment for different phenotypes? (2020) Intensive Care Medicine; DOI: 10.1007/s00134-020-06033-2
[4] Tran K, Cimon K, Severn M, Pessoa-Silva CL, Conly J (2012) Aerosol Generating Procedures and Risk of Transmission of Acute Respiratory Infections to Healthcare Workers: A Systematic Review. PLoS ONE 7(4): e35797. doi:10.1371/journal.pone.0035797
[5] Alhazzani W, Moller MH, Arabi YM, et al. Surviving Sepsis Campaign: Guidelines on the Management of Critically Ill Adults with Coronavirus Disease 2019 (COVID-19). Critical care medicine. 2020;PREPUBLICATION.
[6] The Australian and New Zealand Intensive Care Society (ANZICS). COVID-19 Guidelines. Version 1. 16 March 2020. https://www.anzics.com.au/wp-content/uploads/2020/03/ANZICS-COVID-19-Guidelines-Version-1.pdf
[7] Leonard S, Atwood CW Jr, Walsh BK, DeBellis RJ, Dungan GC, Strasser W, Whittle JS, Preliminary Findings of Control of Dispersion of Aerosols and Droplets during High Velocity Nasal Insufflation Therapy Using a Simple Surgical Mask: Implications for High Flow Nasal Cannula, CHEST (2020), doi:https://doi.org/10.1016/j.chest.2020.03.043.
[8] Williams R, Rankin N, Smith T, Galler D, Seakins P. Relationship between the humidity and temperature of inspired gas and the function of the airway mucosa. Critical care medicine. 1996;24(11):1920-1929.
[9] Miller TL, Saberi B, Saberi S (2016) Computational Fluid Dynamics Modeling of Extrathoracic Airway Flush: Evaluation of High Flow Nasal Cannula Design Elements. J Pulm Respir Med 6:376. doi: 10.4172/2161-105X.1000376. (Bench, Prospective, Not Randomized) https://www.omicsonline.org/open-access/computational-fluid-dynamics-modeling-of-extrathoracic-airway-flush-evaluation-of-high-flow-nasal-cannula-design-elements-2161-105X-1000376.php?aid=81462
[10] Thille, A.W. et al. Effect of Postextubation High-Flow Nasal Oxygen With Noninvasive Ventilation vs High-Flow Nasal Oxygen Alone on Reintubation Among Patients at High Risk of Extubation Failure: A Randomized Clinical Trial. JAMA. 2019 Oct 2;322(15):1465-1475. doi: 10.1001/jama.2019.14901.
[11] Doshi, Pratik et al. High-Velocity Nasal Insufflation in the Treatment of Respiratory Failure: A Randomized Clinical Trial. Annals of Emergency Medicine, 2018. Published online ahead of print. https://www.ncbi.nlm.nih.gov/pubmed/29310868
[12] Doshi, P. et al. The ventilatory effect of high velocity nasal insufflation compared to noninvasive positive-pressure ventilation in the treatment of hypercapneic respiratory failure: A subgroup analysis. Heart & Lung 000 (2020) 16. https://doi.org/10.1016/j.hrtlng.2020.03.008