Treating PTSD Patients in Respiratory Distress—How to Manage the Mask Intolerance?

Two well-known things about non-invasive positive pressure ventilation (NiPPV) are that:
- It is the gold standard for initial non-invasive respiratory distress treatment, especially resulting from COPD and
- It fails up to a third of the time because of the patients’ mask intolerance[1]
This puts clinicians in a difficult spot when they are faced with a patient in respiratory distress who also has post-traumatic stress disorder (PTSD). Although not all PTSD patients are going to fail NiPPV treatment, they are especially likely to have psychiatric comorbidities that include anxiety or depressive disorders[2], conditions that may make a tightly fitting face mask pushing pressure into your lungs hard to tolerate.
While there isn’t much literature specifically on the association between PTSD and the likelihood of failing NiPPV in the Emergency Department, there is literature on PTSD and treating Obstructive Sleep Apnea(OSA) with CPAP—another mask-based, pressure-based respiratory modality. A meta-analysis of the OSA literature by Zhang et al showed that patients with PTSD and OSA had significantly lower adherence to CPAP therapy by comparison to patients with OSA alone.[3]
It’s important to note that we can’t ascribe this increased lack of compliance specifically to mask-intolerance alone. This population has a constellation of neurocognitive and physiologic symptoms that contribute to the outcome the meta-analysis found. Clinicians who frequently work with veterans and other groups experiencing PTSD, know that management of these complex patients is challenging. They may have a hard time successfully treating some of these patients with NiPPV. So, what are some options?
Sedation or Restraints

When the discomfort of a mask turns more intense and becomes anxiety or claustrophobia, coaching a patient through it may not work. Clinicians may then have to face the decision of whether or not to sedate the patient, or even put them in restraints. That option is of course not without consequence.
Restraints can be frightening and uncomfortable, especially if a patient is already experiencing anxiety. And sedation might even contribute to PTSD following ICU stays. Parker et al report in their paper Posttraumatic Stress Disorder in Critical Illness Survivors: A Metaanalysis that the prevalence of PTSD development was higher among critical illness survivors who had undergone sedation with benzodiazepines.[4] Similar, “early memories of frightening ICU experiences” also was listed as a factor contributing to higher prevalence. In essence, these options might be retraumatizing to some PTSD patients.
Intubation
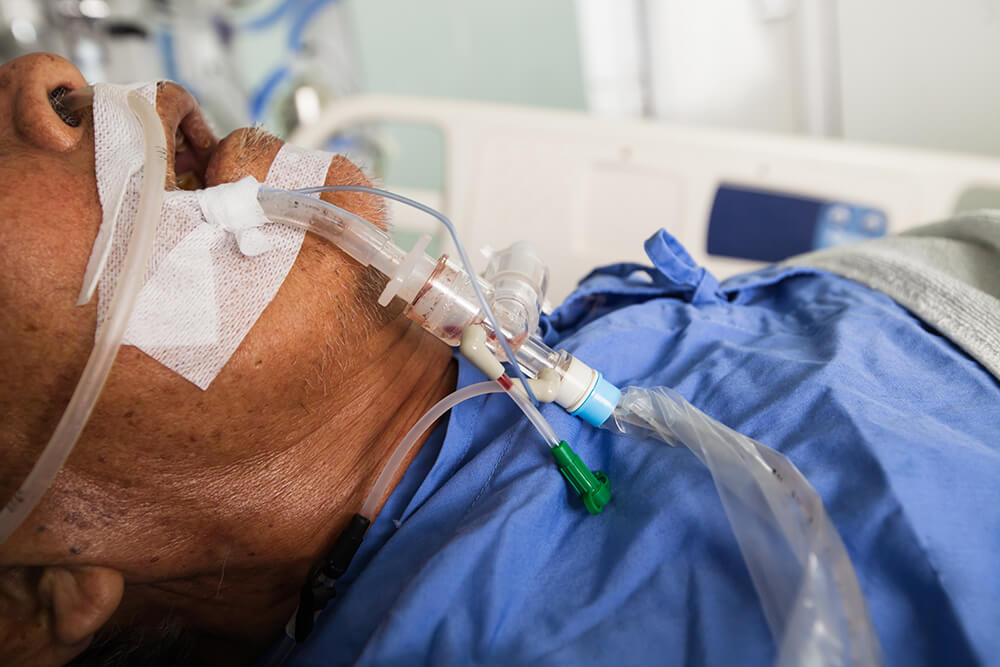
If a sick patient fails on NiPPV and is deteriorating quickly, there often is no other recourse than intubation. However, intubations can sometimes be life-threatening medical crises in and of themselves, though their risks are generally reduced when performed by experienced doctors.[5] Even when done successfully, they require sedation and can be frightening. The procedure is also an escalation of care and costly for the hospital and should therefore be avoided when possible.
Mask-Free Alternative to NiPPV

One way to potentially avoid intubation due to failure of noninvasive ventilation modalities is using Vapotherm high velocity therapy which is a mask-free alternative to NiPPV. There is no increased risk of intubation using high velocity therapy in place of NiPPV.[6] It may provide a useful tool, particularly for those patients where the clinician wishes to avoid mask-based NiPPV therapy due to contraindications or tolerance, such as the PTSD patient population.
High velocity therapy gives patients the ventilatory support of NiPPV with the comfort of humidified high flow. They can comfortably eat, speak, drink, and take oral medication—factors that may be appreciated by all patients, but especially those unable to tolerate tightly sealed masks. If your PTSD patients in respiratory distress do fail on NiPPV, find out whether your hospital has high velocity therapy and see if you can help them that way.
No Mask. No Problem. Mask-Free NIV
REFERENCES
[1] Carron M. et al. Complications of non-invasive ventilation techniques: a comprehensive qualitative review of randomized trials. British Journal of Anaesthesia. 110(6):896-914. (2013) https://www.ncbi.nlm.nih.gov/pubmed/23562934
[2] Brownlow, Janeese A., Gerlinde C. Harb & Richard J. Ross. Treatment of Sleep Disturbances in Post-Traumatic Stress Disorder: A Review of the Literature. Curr Psychiatry Rep (2015) 17: 41
DOI 10.1007/s11920-015-0587-8
[3] Zhang, Ye, Jason G. Weed, Rong Ren, Xiangdong Tang, Wei Zhang. Prevalence of obstructive sleep apnea in patients with posttraumatic stress disorder and its impact on adherence to continuous positive airway pressure therapy: a meta-analysis. Sleep Medicine 36 (2017) 125e132.
[4] Parker, Ann M, Thiti Sricharoenchai, Sandeep Raparla, Kyle W. Schneck, O. Joseph Bienvenu, Dale M. Needham, Posttraumatic Stress Disorder in Critical Illness Survivors: A Metaanalysis. Crit Care Med. 2015 May;43(5):1121-9. doi: 10.1097/CCM.0000000000000882.
[5] Divatia, Jigeeshu V, Parvez U Khan, and Sheila N Myatr. Tracheal intubation in the ICU: Life saving or life threatening? Indian J Anaesth. 2011 Sep-Oct; 55(5): 470–475. doi: 10.4103/0019-5049.89872
[6] Doshi, Pratik et al. High-Velocity Nasal Insufflation in the Treatment of Respiratory Failure: A Randomized Clinical Trial. Annals of Emergency Medicine, 2018. https://www.ncbi.nlm.nih.gov/pubmed/29310868