Researchers Publish Approach to High Flow Nasal Cannula in Neonates
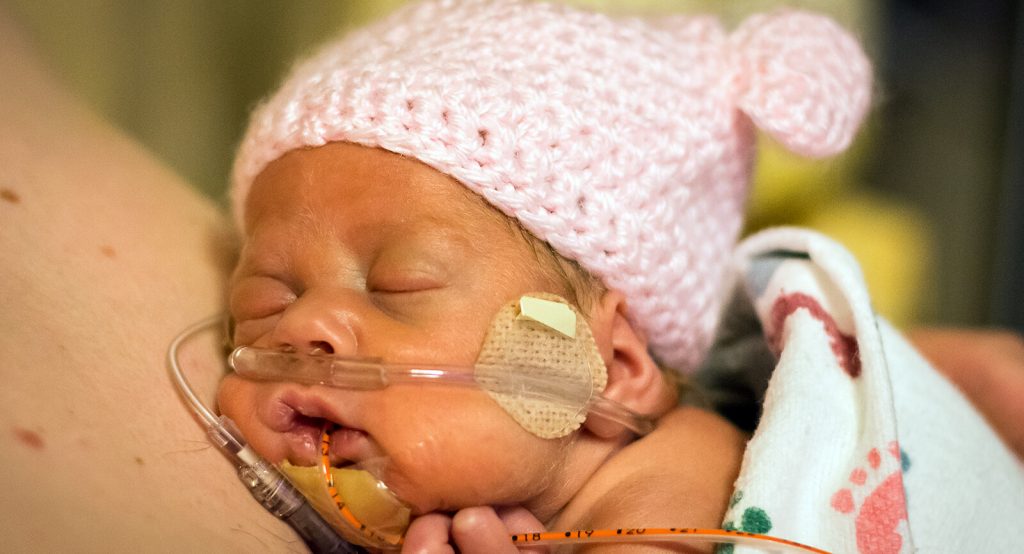
High flow nasal cannula (HFNC) is commonly used to support neonates with respiratory distress syndrome (RDS), but reports suggest there is a wide variation in clinical practice management using this therapy. In an effort to identify consensus on the approach to HFNC in neonates, Dr. Brad Yoder surveyed 7 of the most experienced HFNC clinicians and researchers in the world. The group then came together to generate an informative discussion around these questions. The results of this process were published on March 23, 2017 in Journal of Perinatology titled Consensus Approach to Nasal High-Flow Therapy in Neonates.[1]
It is important to note that the approach did not distinguish between the use of High Velocity Nasal Insufflation (HVNI) and commodity high flow oxygen products (HFNC). While both HVNI and HFNC use a cannula interface and L/min parameters, there are differences in design elements as well as clinical outcomes between the two modalities. They also fall under different FDA product categories. However, there is no reason to believe that the consensus reached in this paper is incorrect for HVNI usage given that only one of the seven physicians used HFNC exclusively. The rest of this piece uses the term HFNC as an umbrella term, though the authors of the paper used the term nasal high-flow therapy (nHFT)–another commonly used phrasing.
The participants of this consensus process were composed of core authors from the most influential HFNC papers from the last several years, including:
Brad Yoder, MD – Department of Pediatrics-Neonatology, University of Utah School of Medicine, Salt Lake City, UT, USA
Brett Manley, MD – The Royal Women’s Hospital, Melbourne, and the Department of Obstetrics and Gynaecology, The University of Melbourne, Melbourne, VIC, Australia
Clare Collins, MD – Mercy Hospital for Women, Melbourne, VIC, Australia
Kevin Ives, MD – John Radcliffe Hospital, Oxford, UK
Amir Kugelman, MD – Bnai Zion Medical Center, Rappaport Faculty of Medicine, Technion, Haifa, Israel
Anna Lavizzari, MD – Fondazione IRCCS Cà Granda, Ospedale Maggiore Policlinico, Università degli Studi di Milano, Milan, Italy
Michael McQueen, MD – Division of Neonatology, Banner Health System, Phoenix, AZ, USA
Some of the key takeaways from the discussion are interpreted here. We encourage all neonatal practitioners to read this important publication.
What gas temperature and gas humidification should be used when using high flow nasal cannula in neonates?
The authors unanimously agreed that HFNC should be delivered with adequate gas heating to maintain 34-37 °C at 100% relative humidity.
While administering high flow nasal cannula, how should the nasal cannula be sized?
The authors agreed that the preferred cannula to nares ratio (i.e. the percent of the nare diameter obstructed by the prong) should be approximately 50%. The group agreed the cannula to nares ratio should never exceed 80%.
What is the maximum flow when using high flow nasal cannula in neonates?
The authors agreed that the maximum flow rate to be used in neonates is 8 L/min.
Is high flow nasal cannula an appropriate tool for support of neonates after extubation?
The authors unanimously agreed that, subsequent to several major clinical trials, current evidence supports the use of HFNC for supporting neonates after extubation as a direct alternative to nasal continuous positive airway pressure (nCPAP).
Is high flow nasal cannula an appropriate tool to transition off nasal CPAP in the neonatal population?
The authors unanimously agreed that current evidence supports the use of HFNC as an alternative noninvasive mode to transition stable infants off nasal continuous positive airway pressure (nCPAP).
Should FiO2 or flow be decreased first when weaning off high flow nasal in the neonatal population?
The authors reached consensus that FiO2 should be weaned first to less than .30 before weaning flow.
What clinical parameters should suggest increasing flow of high flow nasal cannula in neonates?
The authors agreed that the approach to escalation (increasing flow) of HFNC should be based on signs of respiratory distress, including work of breathing and FiO2.
What gas flow rate should be used when starting high flow nasal cannula?
Most authors agreed that initial gas flow should be in the range of 4-6 L/min when initiating HFNC in the neonatal population. However, two authors had different approaches, one initiated flow at 8 L/min in all cases, while the other was more conservative with initial flow.
What clinical parameters should suggest decreasing flow of high flow nasal cannula in neonates?
The authors recommend flow should be decreased in 0.5-1.0 L/min increments when patient shows stable FiO2 and indices of work of breathing.
What clinical parameters should suggest changing from high flow nasal cannula to other NIV mode?
The authors suggest that clinicians should consider changing to alternative modes of NIV, if
- Elevated FiO2 requirement greater than .40 to maintain target SpO2
- Consistent increased work of breathing
- Excessive or severe apnea events
Is high flow nasal cannula an appropriate primary therapy for neonates with suspected surfactant-deficient RDS?
There was general agreement, though not unanimous, regarding the use of HFNC as primary support for surfactant-deficient RDS. Five of the seven authors believed using HFNC as primary support was warranted, while two were unconvinced. One of the authors who agreed with the use as primary support offered qualifications based on gestational age and FiO2 requirement.
At what flow rate should high flow nasal cannula be discontinued in the neonatal population?
The authors did not reach agreement on when to stop high flow nasal cannula. They do agree that this area warrants further clinical investigation. The authors discontinue high flow nasal cannula at flow rates between 1 L/min and 4 L/min.
These guidelines can be a useful resource for neonatal intensive care units to construct or modify clinical protocols.
To review the full article, visit Journal of Perinatology – Consensus Approach to Nasal High-Flow Therapy in Neonates
Learn more about neonatal HFNC best practices
REFERENCES
[1] Yoder BA, B Manley, C Collins, K Ives, A Kugelman, A Lavizzari, and M McQueen. “Consensus approach to nasal high-flow therapy in neonates.” Journal of Perinatology (2017) 00, 1–5.